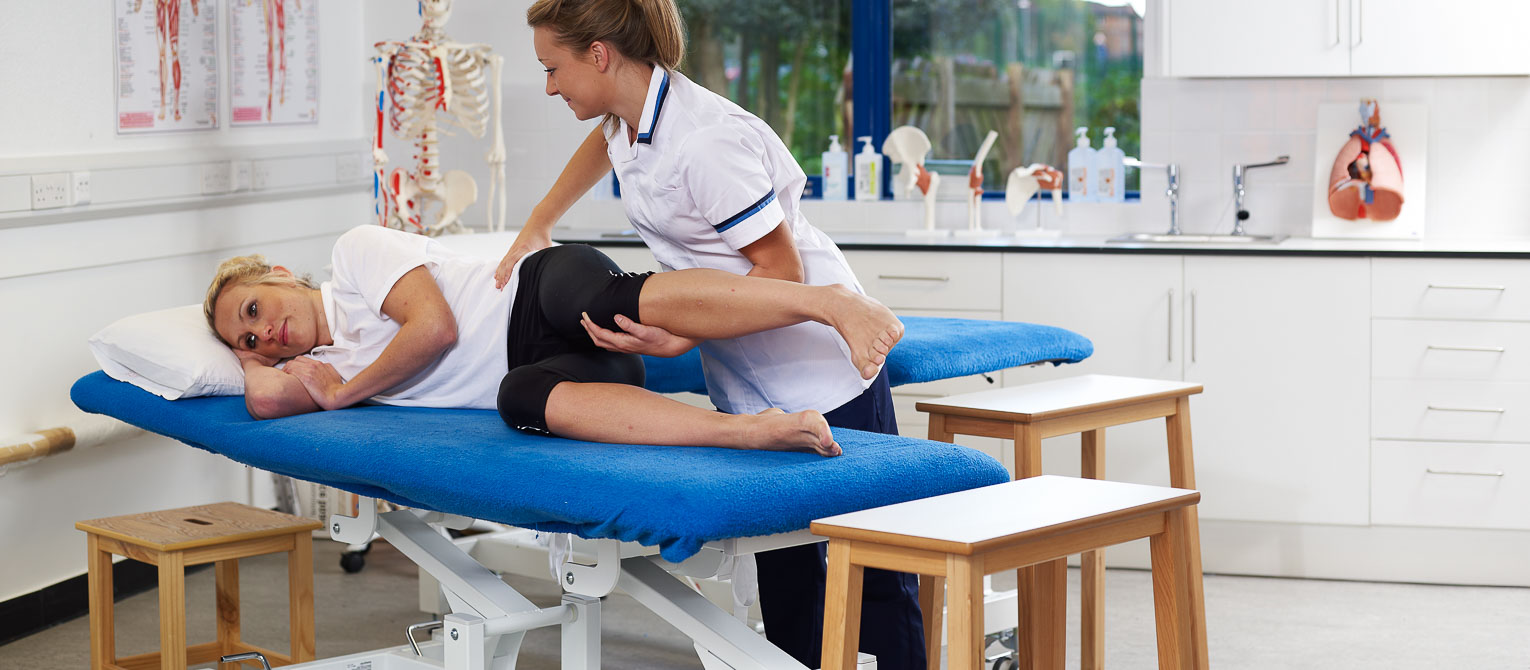
Our curriculum ensures students learn the appropriate clinical and communications skills in preparation for meeting patients. With excellent access to clinical resources and working professionals both in the community and hospitals, as well as in our brand-new medical building. Our course will equip you with all the skills, knowledge and practical experience required to pass the licensing examinations and for a rewarding career.
Accreditation
This course is designed to meet General Medical Council (GMC) educational standards and according to the requirements of the Faculty of Physician Associates (FPA). This ensures that our graduates are prepared for the GMC Physician Associate Registration Assessment examination which demonstrates that they are competent and safe to practise.
University of the Year finalist
Recognised for our graduate success, we’re shortlisted for University of the Year in the Times Higher Education Awards 2025.
Overview
The course is a well-established two-year postgraduate education programme, which equips you with the relevant knowledge, develops your clinical capabilities, competencies, and reasoning to work across 20 specialty areas in the UK, such as internal medicine, general practice, surgery and emergency medicine.
You will develop key skills to be able to work within multiprofessional healthcare teams supporting clinical specialists. You will be trained according to the medical model, and learn how to diagnose common conditions, formulate patient healthcare management plans, and understand when to refer patients and ask for help.
Your learning will include a mixture of campus-based activity such as lectures, seminars, face-to-face tutorials, skills lab training and communication skills, as well as clinical placements.
During placements you will be carefully supervised, develop key interpersonal skills with patients and colleagues, and work collaboratively with your clinical supervisor and other healthcare professionals to manage patient care.
On successful completion of the course, you’ll be able to take the national Physician Associate Registration Assessment (PARA), which allows you to register with the General Medical Council and work as a physician associate in the NHS.
Placements
Practice learning experiences are in primary, secondary care and voluntary environments, including GP practices, hospitals, hospices, community hospitals and other out-patient and community settings. In the first year of the course, you will undertake one-day-a-week placements in primary care, A&E and out-patient departments from January to August. These are based predominantly in Three Counties of Worcestershire and Herefordshire and Gloucestershire.
The second year is mostly placement based with four weeks of academic in-days, some on a Friday. You will be assigned to acute hospital Trusts or primary care and rotate through a rich variety of different specialties. Your second year will therefore involve travel and experiencing longer periods of placement attachments.
Course content
Our course is student-centred and informed by the latest research and developments in the field, as well as feedback from students and employers. Therefore, modules do occasionally change to keep the course up-to-date and relevant.
All modules are mandatory to ensure you’re properly prepared for your future career in the clinical environment. Successful completion of year 1 is required to progress to year 2 and the dissertation module.
We regularly review our courses to reflect the latest research and developments in the subject area, as well as feedback from students, employers and the wider sector. As a result, modules may change to ensure the course remains current and relevant.
Careers
Physician associates are part of the ‘medical associate professions’ grouping in the health and care workforce and were established in the UK since 2003. The University of Worcester’s MSc Physician Associate course was introduced in 2016 and so we have had many years’ experience of graduating students. Our graduates work within the NHS in multidisciplinary healthcare teams always under the supervision of a doctor.
Physician associates are highly skilled, well-paid professionals with many employment opportunities. Following licensing and registration with the General Medical Council your generalist skills allow you to work in a GP surgery, or be based in a hospital, but wherever you work, you will have direct contact with patients.
There is a significant demand for physician associates within the healthcare workforce.
- Once qualified, you could work in a hospital, or a GP surgery.
- You might move from general or emergency care into a specialism like paediatric care or mental health.
- As an experienced physician associate you might be able to move into management, medical teaching, or research.
- You may also choose to apply for Graduate Entry Medicine and train as a doctor.
Course highlights
Teaching and assessment
You’ll be taught through a combination of structured lectures, clinical simulations, directed and independent study, and group and individual tutorials. There’ll be lots of opportunities to hone your clinical skills through simulated learning including skills sessions using a range of simulation manikins.
Your assessments will help prepare you for your future career, and include assessed simulation, reflective case portfolios, research proposals, and placement observation.
Teaching and assessment contents
You are taught through a combination of structured lecturers, clinical simulation, recorded material with supporting seminars, case-based learning, directed and independent study, group and individual tutorials, with the additional support of e-learning strategies using the virtual learning environment. There will be input from other agencies, service users and professionals as appropriate.
The first year of the course aims to lay down a foundation of knowledge about key illnesses and diseases, their pathophysiology, presentation, diagnosis, treatment and management, as well as providing a safe environment to learn and practice history taking, clinical examination and skills.
Year 2 is mainly set in clinical practice with regular academic days in the University. Practice learning experiences are clinical placements in primary and secondary care environments, including GP practices, hospitals, hospices, community hospitals and other out-patient and community settings. These are based predominantly in the Worcestershire, Herefordshire, Gloucestershire, Oxfordshire and Warwickshire.
Entry requirements
Applicants should normally have GCSE (or equivalent) in Maths and English at grade C/4 or above, plus one of the following:
- 2:1 honours degree or above in a relevant health or life science, and 150 hours of health or care experience.
- 2:1 honours degree or above in social work, or a physical science with completed degree level biology modules, and 150 hours of health or care experience.
- 2:2 honours degree or above in a relevant life sciences subject (to include a transcript with no more than 4 modules graded at less than 50%) with 300 hours of health or care experience.
Any questions?
If you have any questions about entry requirements, please call our Admissions Office on 01905 855111 or email admissions@worc.ac.uk.
Fees
Fees contents
UK students
In 2026/27 the standard tuition fee for full-time UK students enrolling on this course is £11,250 per year.
Tuition fees are reviewed annually and may increase each year for both new and continuing students.
For more details on course fees, please visit our course fees page.
How to apply
How to apply contents
Applying through UCAS
UCAS is the central organisation through which applications are processed for full-time undergraduate courses in the UK.
Read our how to apply pages for more information on the application process, or if you’d like to apply for part-time study.
Contact
If you have any questions, please get in touch. We're here to help you every step of the way.
Admissions Office
admissions@worc.ac.uk01905 855111More to explore
Open Days
Visiting us is the best way to get a feel for student life at the University of Worcester.

The City of Worcester
Worcester is a welcoming university city with great transport links and plenty of student parking.

Accommodation
Benefit from our accommodation guarantee. We have rooms on campus to suit every budget including en-suite options.